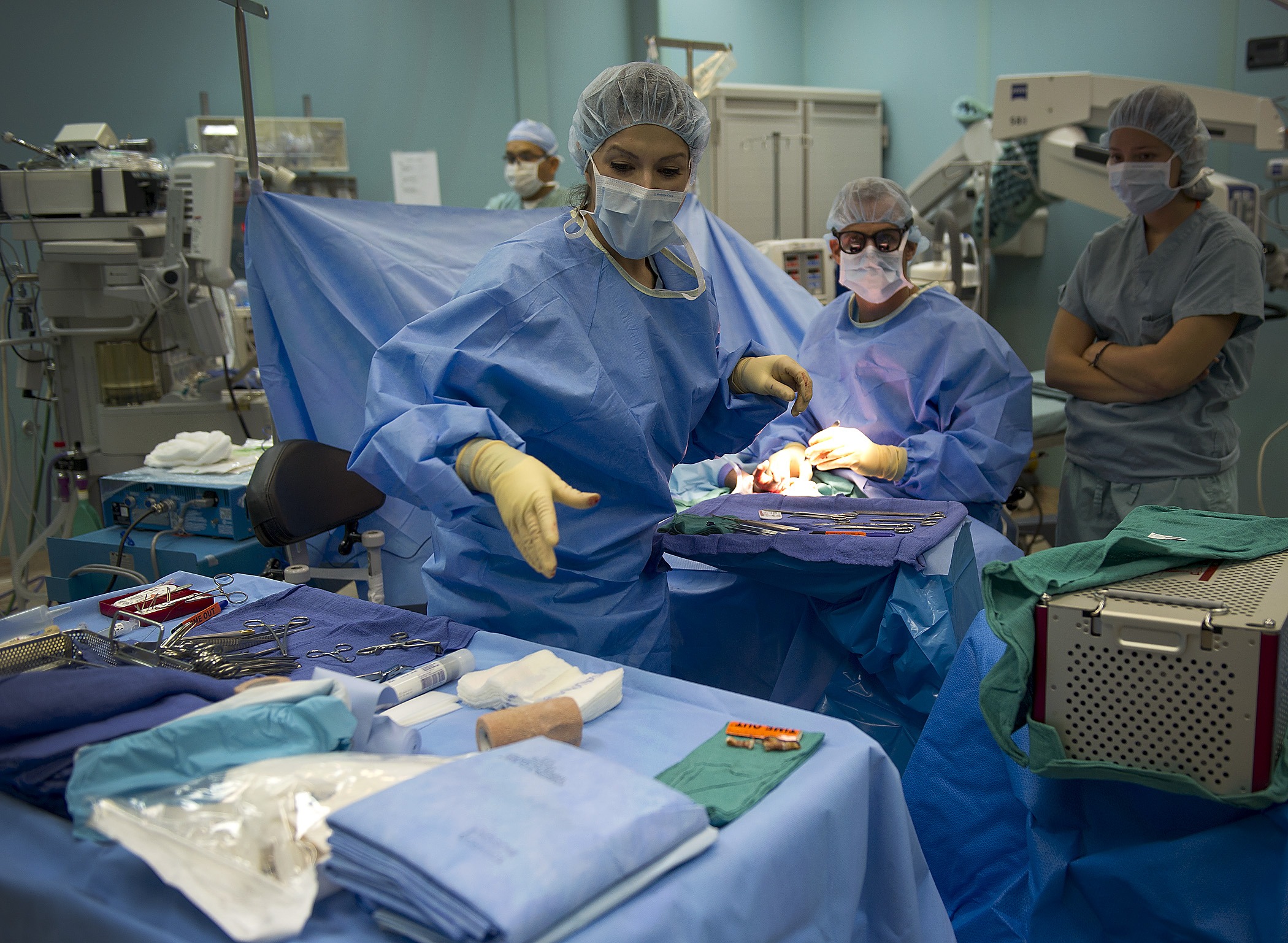
Technology has infiltrated every aspect of the healthcare system. And in some cases, the resulting new medical applications are allowing us to peer deeper into one of the most mysterious organs in the human body.
An artificial intelligence (AI)-enabled technology published in the Nature Medicine journal is improving the extremely precise and sensitive field of brain surgery where it matters most: in the operating room (OR). It’s enabling brain surgeons to diagnose brain tissue and tumors faster than and as accurately as pathologists.
How This New AI Helps in the OR
How can a trained surgeon diagnose tissue abnormalities as well as a trained pathologist? AI and advanced imaging techniques are applied to tissue samples taken from the patient, while the patient is still on the operating table, to guide the next steps in the surgery and the treatment plan.
Traditionally, surgeons cut the tissue and send it to the lab, which freezes and stains it to look at it in the microscope. This whole process takes around 30 minutes or longer. But with the new AI technology, freezing and staining are not required; as a result, the time gets cut drastically to two and a half minutes. The tissue is still cut from the patient, but lasers are used to create images, and a computer reads the images in front of the surgeons on a TV in the OR.
Daniel A. Orringer is a neurosurgeon in New York City-based N.Y.U. Langone Health center, and a contributor to the report of the new technology. He says that although MRI scans taken before the operation help surgeons gain footing on what’s going on in the patient’s brain, diagnosis through tissue sample is the most concrete justification for brain surgery.
This new process not only speeds up the previous methods, but it can also catch details that the previous processes can easily miss. For example, he says, the spread of a tumor along nerve fibers can be identified with this technique. Additionally, the tissue doesn’t get destroyed by the freezing and staining processes; it can be saved or reused for more testing.
Myriad Applications for This Medical AI
The new technology can be applied to any procedure where the physician needs to biopsy and analyze tissue during surgery, including breast, skin, head and neck, and gynecology. The report mentioned the shortage of neuropathologists (pathologists who specialize in analyzing brain tissue), but this tool can help fill the void.
Joshua Bederson is the chairman of neurosurgery at Mount Sinai Health System; he says that this innovative method of analyzing tissue is going to be “very useful”, and it’s highly probable that the authors of this paper understated the true potential of this new tool.
In some hospitals, he says, brain surgeons don’t even order frozen tissue analysis because they don’t trust them in comparison to tissue analyzed after the surgery. It can take weeks, not hours, to analyze brain tissue, he said, adding that the neuropathologists he works with are “outstanding. They don’t want us to make life-altering decisions based on [frozen sections, which are] not so reliable.”
The report used experts at medical centers known for their excellence in neuropathology and neurosurgery, making the accuracy of frozen section analysis much higher than the national average.
278 patients’ brain tissues were analyzed during surgery. Each sample was split into two: one went into the computer system for AI analysis, while the other was sent to the neuropathologist. Diagnoses were compared post-operation, and the AI just marginally out-performed the humans, with AI at a 94.6% accuracy rate and humans at a 93.9% accuracy.
Still Some Room for Improvement
The process generates virtual images comparable to traditional slides that humans can study from and examine on demand.
To train the AI algorithm, the researchers fed it tissue images from 415 brain surgery patients. The goal was to have the AI identify the 10 most common types of brain tumors. For samples that the AI couldn’t diagnose due to not having enough data for training (for the rarest cases of brain cancer), the system threw out those samples.
The system did misdiagnose 14 cases that humans caught, but then again, the doctors missed 17 cases that the AI got right. Overall, in a field that’s not as specialized as neurosurgery and neuropathology, these are extremely negligible numbers.
Orringer says he’s excited about the amazing results. The research culminated in the right combination of an AI algorithm with human intuition that performed as well as human doctors do. In his own office, Orringer uses the algorithm to determine whether he needs to cut more brain tissue or if the most recent sample shows a stop in the spread of tumor cells. It decreases the amount of time a patient is under anesthesia, which in turn greatly reduces the risk of complications during surgery.
Orringer says this technology enables him to save so much time, often “six multiplied by 30 or 40 minutes.”
Applying AI Internationally
Bederson says he has participated in a pilot study of a similar research program. He says his hospital system is considering acquiring the technology, and he’s looking forward to using it in his own practice.
He added that this new AI application “won’t change brain surgery, but it’s going to add a significant new tool, more significant than they’ve stated.”
What do you think of this new AI development? Would you trust it? Or do you prefer the old-fashioned way? As always, let us know your thoughts in the comments below!